Key messages
When compared to other industries, workers in the healthcare and social assistance industry are at a much greater risk of exposure to biological hazards because of the nature of their work providing care to people who may be unwell, providing support to people with complex conditions, and handling of potentially infectious materials. However, the risk of biological hazards can be effectively managed in the workplace with preventative controls.
Jump to:
How you should identify and assess hazards and risks How you should control risks Case study: Norovirus outbreak in an aged care home
How you should identify and assess hazards and risks
Consult with workers and others to identify and assess hazards and risks
Identifying the different sources of biological hazards (where they can be found) and how they can affect people (including whether they can spread to others) is the first step of your risk assessment.
When identifying the hazards and potential infection sources consider the following factors which may increase risks:
How you should control risks
Consult with workers and others to design controls
Eliminate the risks of biological hazards as much as you reasonably can, including through good work design. The hierarchy of controls can assist you in managing risks.
In some settings, relatively simple control measures may effectively minimise the risk (e.g. PPE suitable to the risk, ventilation, good hygiene practices, regular cleaning).
Additional control measures may be required in settings where risks are higher (e.g. infectious disease wards, aged care homes where residents are especially vulnerable to disease, during outbreaks).
In these circumstances, consider:
- increased hand hygiene
- more frequent cleaning and disinfection
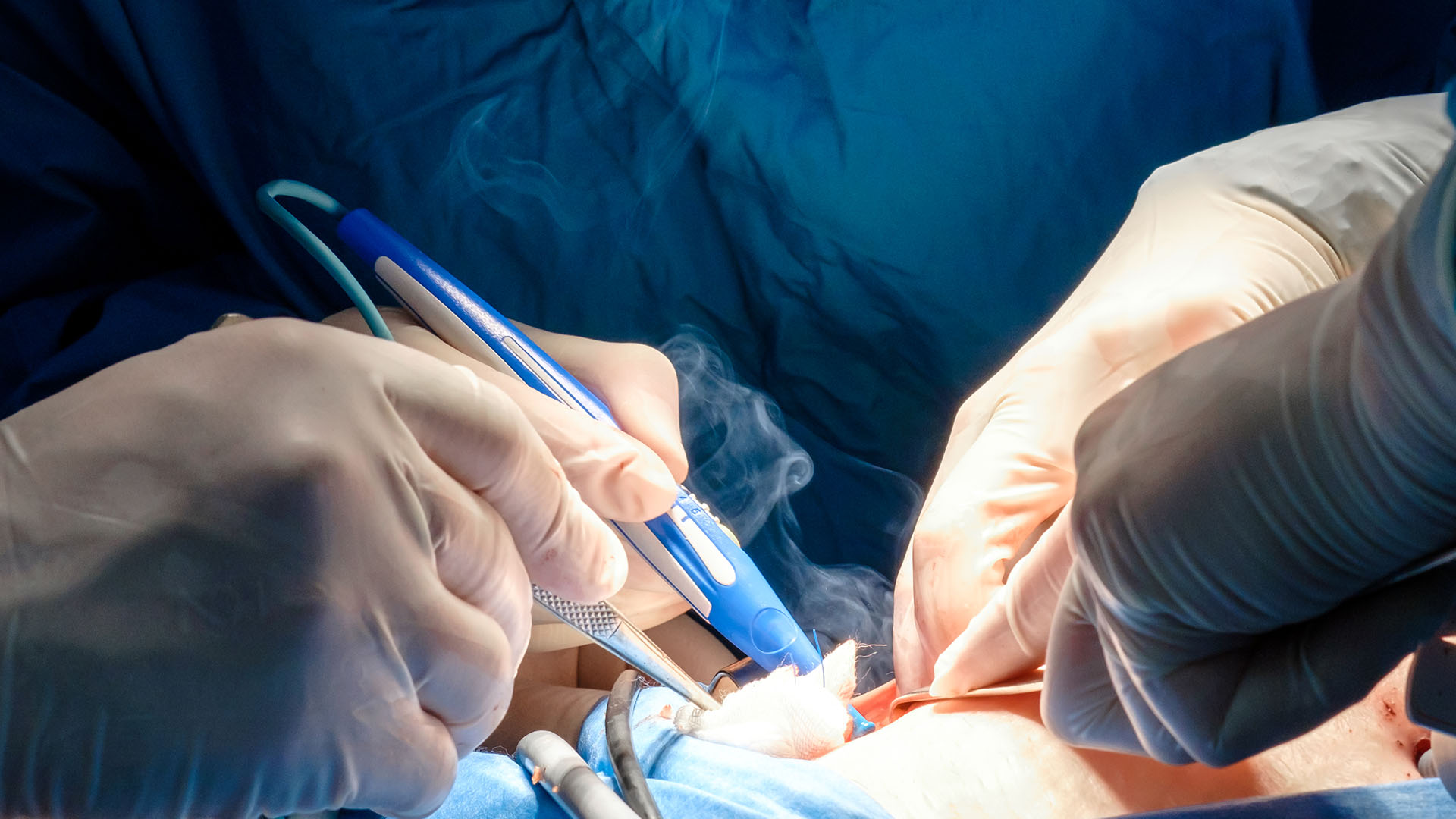
- improved ventilation (e.g. surgical plume evacuator system, HEPA filters)
- use of negative pressure rooms
- signage on patient or client rooms
- greater physical distancing
- testing of visitors
- isolation of infected people from others (e.g. use an isolation room or cohort infectious patients together), and
- use of portable medical tents.
It is important that you seek and monitor information and advice from authoritative sources relevant to your workplace to help you identify the most effective and reliable control measures, particularly if there are outbreaks or emerging hazards.
Maintain and review controls to ensure they are being used and are effective, especially after any changes to the task or workplace.
In addition to the general advice on when to review risk controls, you should also consider reviewing controls when you receive new information about a biological hazard (e.g. a new virus or strain of an existing virus) or ways to control risks (e.g. a new vaccine developed).

Case study – Norovirus outbreak in an aged care home
A resident in an aged care home reports they have been unwell for over a day with diarrhoea and that they have been in the communal dining room as well as some group activities. A swab later reveals that the resident has a norovirus infection. The aged care home’s policy requires the immediate use of additional control measures during infectious disease outbreaks to limit the spread between people.
The aged care home’s policies require additional contact measures to be put in place right away, with workers practicing more frequent hand hygiene and using masks, gloves and gowns.
Unfortunately, the aged care home cannot confine all residents to their rooms as there are not enough staff to monitor them all or manage restriction zones. After checking all the residents, 2 more report diarrhoea and vomiting. The residents with symptoms are provided with appropriate care and support in their rooms, which have ensuites, to prevent interaction with other residents while they are infectious.
While workers have increased handwashing and use of PPE, other staff at the home (including cleaning staff and cooks) are not given additional training or access to equipment. Investigation also reveals low levels of hand hygiene among residents and a lack of routine cleaning in dining areas. The virus spreads to 6 more people, including 3 workers, before it is finally contained.
An education program is developed to assist in preventing further infections. In future outbreaks, cleaning staff and cooks are given training in hand washing, issued with PPE, and asked to report symptoms promptly. Procedures are also updated to increase cleaning of frequently touched surfaces to reduce the risks of environmental contamination and transmission.